La terapia fotodinámica I-PDT con láser Multidiode™ 630 PDT de INTERmedic ofrece una solución a las personas que sufren hidrosadenitis supurativa y carcinoma basocelular, entre otras patologías.
La terapia fotodinámica láser I-PDT es una solución láser mínimamente invasiva que resuelve estas patologías en pocas sesiones, sin cirugía, sin hospitalización y sin baja laboral. Efectiva, cómoda y con resultados estéticos excepcionales, esta nueva técnica de tratamiento mejora de forma notable la calidad de vida de los pacientes y les ofrece una esperanza de curación, según se desprende de los excelentes resultados registrados hasta el momento, en diferentes estudios clínicos. En este artículo, repasamos en que consisten estas tres patologías y cuales son las ventajas que aporta el tratamiento con terapia fotodinámica I-PDT, respecto al abordaje convencional con técnicas de tratamiento tradicionales como la medicación oral o la cirugía.
Carcinoma basocelular o basalioma
¿Qué es? Es un tipo de cáncer de piel frecuente a partir de los 50 años. Suele aparecer en las zonas del cuerpo más expuestas a la radiación solar (manos, cara, cuello y escote). Puede presentarse en forma de nódulo o úlcera, que puede llegar a sangrar. El diagnóstico de carcinoma basocelular se confirma mediante biopsia. La detección precoz y el crecimiento lento de este tipo de tumores hacen que se puedan tratar de forma efectiva en la mayoría de los casos.
¿Quién lo trata? Dermatólogo y Cirujano Plástico.
Abordaje convencional. Según el tamaño del tumor y su localización se realiza extirpación completa mediante cirugía convencional o cirugía de Mohs (eliminando el tumor capa a capa tras verificación). En lesiones pequeñas, se usa crioterapia y fármacos tópicos inmunomoduladores.
Terapia fotodinámica láser I-PDT. La terapia fotodinámica elimina tumores de gran tamaño, superficiales y profundos, sin necesidad de recurrir a la cirugía, sin cicatrices y de forma cómoda y efectiva.
 Fotos cortesía del Dr. Manuel Ángel Rodríguez Prieto. Dermatólogo. Hospital de León (León)
Fotos cortesía del Dr. Manuel Ángel Rodríguez Prieto. Dermatólogo. Hospital de León (León)
Hidrosadenitis supurativa
¿Qué es? Es una enfermedad inflamatoria crónica y autoinmune que se caracteriza por la aparición de nódulos, forúnculos y fístulas en las glándulas apocrinas de axilas, ingles, nalgas y zona genital. Afecta casi a medio millón de personas en España, pero la mayoría de la población no la conoce. La hidradenitis supurativa es difícil de diagnosticar, de tratar y no tiene solución definitiva por el momento.
¿Quién la trata? El Dermatólogo.
Abordaje convencional. Incluye medicación oral (retinoides, antibióticos e inmunosupresores con efectos secundarios no deseados), inyecciones de corticoides y terapia biológica, de resultados lentos y coste elevado.
Terapia fotodinámica láser I-PDT. Es una terapia mínimamente invasiva, rápida, cómoda y asequible tanto para el médico, como para el paciente. Consiste en inyectar un fotosensibilizante en la zona de la lesión e irradiar con láser de 630nm desde el interior. Estudios realizados en el Hospital de León constatan una clara mejoría de los pacientes tratados de hidrosadenitis supurativa con una sola sesión de I-PDT.
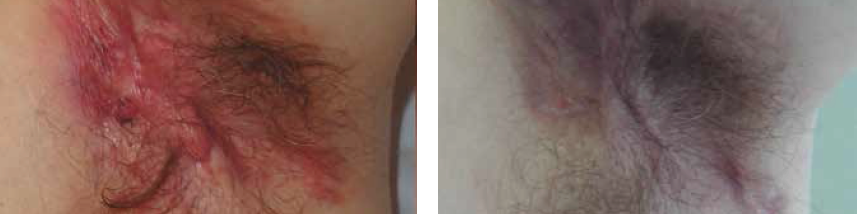 Fotos cortesía del Dr. Manuel Ángel Rodríguez Prieto. Dermatólogo. Hospital de León (León)
Fotos cortesía del Dr. Manuel Ángel Rodríguez Prieto. Dermatólogo. Hospital de León (León)
Fístula anal / colorrectal
¿Qué es? La fístula anal o colorrectal es una lesión en forma de canal en la zona anal que se comunica con la piel, la vagina o la vejiga. Provocada por una herida, una infección o inflamación, sus síntomas son dolor agudo, picor, escozor, sangrado y supuración de heces. En ocasiones puede llegar a producirse un absceso.
¿Quién la trata? El Cirujano General y el Proctólogo.
Abordaje convencional. El tratamiento tradicional pasa por la cirugía, con los riesgos implícitos en cualquier intervención quirúrgica (anestesia, infección) y también la posibilidad de aparición de efectos secundarios como incontinencia de heces.
Terapia fotodinámica láser I-PDT. El objetivo de la terapia fotodinámica láser en fístulas anales es favorecer la cicatricación de ese canal, eliminando el tejido epitelial y favoreciendo su cierre. Induce la necrosis selectiva sin dañar los tejidos adyacentes.
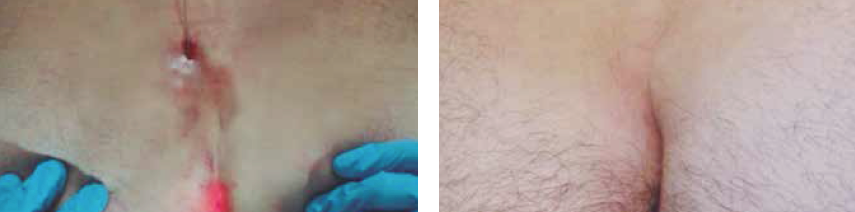 Fotos cortesía del Dr. Manuel Ángel Rodríguez Prieto. Dermatólogo. Hospital de León (León)
Fotos cortesía del Dr. Manuel Ángel Rodríguez Prieto. Dermatólogo. Hospital de León (León)

